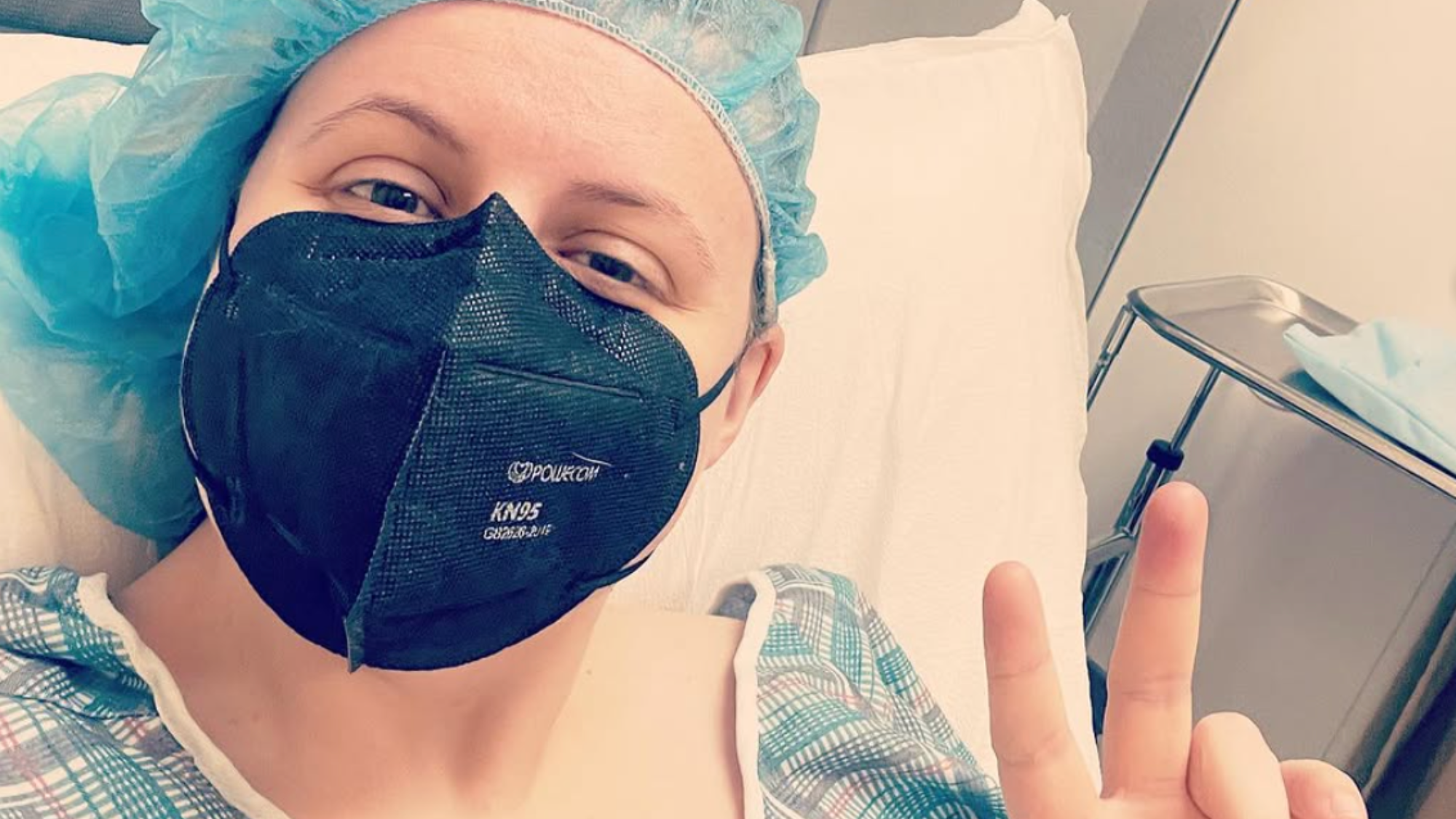
I'm sitting in a hospital bed at 2 AM, wearing one of those gowns that opens in the back, watching my belly expand like I'm six months pregnant. Except I'm not pregnant — I just had my egg retrieval three days ago, and my ovaries have decided to throw the world's worst tantrum.
This is moderate OHSS, and I had absolutely no idea how serious it could get.
Listen, when my clinic mentioned ovarian hyperstimulation syndrome during my IVF consent process, it felt like one of those "rare side effects" you hear about in drug commercials. You know, the ones you tune out because obviously that won't happen to you. Well, plot twist: it happened to me, and I was completely unprepared for how scary it would be.
Here's everything I wish someone had told me about OHSS symptoms in IVF — what it actually feels like, when to worry, and when to get your ass to the emergency room.
What Actually Is OHSS?
OHSS happens when your ovaries get overstimulated from fertility medications and basically go haywire. Instead of just releasing eggs like good little ovaries, they start leaking fluid into places where fluid definitely shouldn't be.
The medical explanation: those follicles that housed your eggs? They release chemicals that make your blood vessels more permeable. Fluid escapes from your bloodstream and pools in your abdomen, chest, and other fun places. Your ovaries also swell up like balloons at a kid's birthday party.
The real-talk explanation: you feel like absolute garbage, and your body does things that make you question everything.
My OHSS Story: When "Mild Bloating" Became a Medical Emergency
After my retrieval in April 2023, I felt pretty good initially. Sure, I was bloated — but they told me to expect that. Day one post-retrieval? Totally fine. Day two? Starting to feel uncomfortable, but I figured it was normal.
Day three is when things went sideways.
I woke up and couldn't button my jeans. Not like "oh, I'm a little puffy" — like, I looked six months pregnant and felt like someone had filled my belly with concrete. I called my clinic, and the nurse said to "monitor it" and come in if it got worse.
How exactly does one monitor concrete belly? I wondered.
By evening, I couldn't eat without feeling nauseous. I was peeing less despite drinking water. And here's the kicker — I was having trouble breathing when I laid flat. That's when my anxiety kicked in because why the hell am I short of breath three days after a routine procedure?
I called the after-hours line, described my OHSS symptoms, and they told me to head to the ER. Not "maybe go if you feel like it" — they said go NOW.
OHSS Symptoms: The Real Talk Version
Mild OHSS Symptoms
- Bloating and abdominal discomfort (think: ate too much Thanksgiving dinner, but it lasts for days)
- Mild nausea
- Weight gain of 2-5 pounds seemingly overnight
- Feeling full quickly when eating
Moderate OHSS Symptoms (What I Had)
- Severe abdominal pain and bloating — I'm talking "can't stand up straight" pain
- Nausea and vomiting
- Rapid weight gain (I gained 8 pounds in 3 days)
- Decreased urination despite normal fluid intake
- Shortness of breath, especially when lying down
- Feeling of fullness or pressure in your chest
Severe OHSS Symptoms (Get to ER Immediately)
- Difficulty breathing or severe shortness of breath
- Chest pain
- Severe abdominal pain
- Vomiting so much you can't keep fluids down
- Little to no urination
- Dizziness or fainting
- Rapid heart rate
Here's the thing about OHSS symptoms in IVF — they can escalate quickly. What feels manageable in the morning can become genuinely scary by evening.
When to Call Your Doctor vs. When to Hit the ER
Call your clinic if:
- You have mild symptoms that are getting gradually worse
- You're not sure if what you're feeling is normal
- You're gaining 1-2 pounds per day
- Your bloating is uncomfortable but not preventing normal activities
Call the after-hours line if:
- Symptoms are progressing rapidly
- You're having trouble eating or drinking
- Your weight gain is more than 2 pounds in 24 hours
- You're feeling short of breath
Go to the ER if:
- You're vomiting and can't keep fluids down
- You're having severe difficulty breathing
- You haven't urinated in 8+ hours despite drinking fluids
- You're having severe abdominal pain
- You feel dizzy or faint
Don't mess around with severe symptoms. I learned this the hard way.
What Happens at the Hospital
When I got to the ER, they took one look at my basketball belly and fast-tracked me. Blood work showed my hematocrit was elevated (meaning my blood was getting thick from fluid loss), and my electrolytes were off.
The ultrasound was honestly terrifying — my ovaries were the size of grapefruits, and there was free fluid floating around my abdomen. The ER doctor explained that in severe cases, they might need to drain the fluid with a needle.
Thanks for that visual, I thought.
I ended up staying overnight for monitoring and IV fluids. They gave me anti-nausea medication and closely watched my kidney function. The scariest part? My oxygen levels kept dropping when I laid flat because the fluid was putting pressure on my lungs.
Not exactly the post-retrieval experience I'd imagined.
The Recovery Reality
Here's what no one tells you about recovering from moderate OHSS: it takes forever. Well, not literally forever, but when you're miserable, two weeks feels like an eternity.
I couldn't do my fresh transfer because my hormone levels were still too high. My body needed time to reabsorb all that fluid and get back to baseline. It took about 10 days before I could wear normal clothes again, and two full weeks before I felt human.
The Easy@Home OPK+HCG tests actually helped me track when my HCG levels finally normalized — which was crucial for planning my eventual frozen transfer.
Who's at Higher Risk?
Looking back, I had several risk factors that should have put OHSS on my radar:
- High AMH levels
- PCOS-like symptoms (though not formally diagnosed)
- Age under 35
- High number of follicles (I had 20 respond)
- Using HCG trigger shot
Women with these risk factors should be extra vigilant about monitoring OHSS symptoms after retrieval.
How to Advocate for Yourself
Here's my biggest takeaway: trust your gut. When I called my clinic on day three saying I felt "really uncomfortable," the nurse initially downplayed it. It wasn't until I specifically said "I'm having trouble breathing" that the tone changed.
Be specific about your symptoms. Don't just say "I don't feel good" — describe exactly what's happening. "I've gained 6 pounds in two days, I'm short of breath, and I can't eat without feeling sick" gets much better attention than "I'm bloated."
And honestly? If you're worried enough to call, you're probably right to be worried.
The Silver Lining (Yes, There Is One)
Despite the drama, my retrieval was actually successful. We got 7 embryos, 5 of which were chromosomally normal. The OHSS didn't affect egg quality — it was just my ovaries being dramatic about the whole process.
And now I'm basically an expert on OHSS symptoms, which makes me a better resource for other women going through IVF. Silver lining: achieved.
Listen, OHSS symptoms in IVF can be genuinely scary, especially when you're not prepared for how intense they can get. But knowing what to watch for — and when to get help — makes all the difference. Don't be a hero. When in doubt, make the call.
This article is for informational purposes only and is not medical advice. Always consult with your healthcare provider about any symptoms you're experiencing.